
Allergic bronchopulmonary aspergillosis
Medical condition / From Wikipedia, the free encyclopedia
Dear Wikiwand AI, let's keep it short by simply answering these key questions:
Can you list the top facts and stats about Allergic bronchopulmonary aspergillosis?
Summarize this article for a 10 year old
Allergic bronchopulmonary aspergillosis (ABPA) is a condition characterised by an exaggerated response of the immune system (a hypersensitivity response) to the fungus Aspergillus (most commonly Aspergillus fumigatus). It occurs most often in people with asthma or cystic fibrosis.[1] Aspergillus spores are ubiquitous in soil and are commonly found in the sputum of healthy individuals. A. fumigatus is responsible for a spectrum of lung diseases known as aspergilloses.[4]
| Allergic bronchopulmonary aspergillosis | |
|---|---|
| Other names | ABPA, Hinson-Pepys disease. |
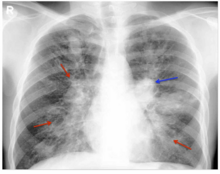 | |
| The chest radiograph of an allergic bronchopulmonary aspergillosis patient shown with left-sided perihilar opacity (blue arrow) along with non-homogeneous infiltrates (transient pulmonary infiltrates indicated by red arrows) in all zones of both lung fields. | |
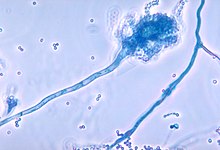 | |
| The conidiophore of the fungal organism Aspergillus fumigatus. | |
| Specialty | Pulmonology, Infectious disease |
| Symptoms | wheezing, coughing, shortness of breath and exercise intolerance.[1] |
| Complications | Asthma exacerbations, aspergilloma, chronic pulmonary aspergillosis, cavitation, local emphysema, chronic or recurrent atelectasis, and honeycomb fibrosis.[2] |
| Causes | Aspergillus exposure. |
| Risk factors | Asthma or cystic fibrosis.[1] |
| Diagnostic method | Chest X-rays, CT scans, blood tests, immunological tests, and sputum cultures.[2] |
| Differential diagnosis | Asthma with fungal sensitivity, cystic fibrosis, bronchiectasis, eosinophilic pneumonia, churg–strauss syndrome, bronchocentric granulomatosis, tuberculosis, and sarcoidosis.[2] |
| Prevention | Corticosteroids and antifungal medications.[2] |
| Medication | Prednisolone and Itraconazole.[2] |
| Frequency | 1–15% of cystic fibrosis patients and 2.5% of adults with severe asthma.[3] |
ABPA causes airway inflammation, leading to bronchiectasis—a condition marked by abnormal dilation of the airways. Left untreated, the immune system and fungal spores can damage sensitive lung tissues and lead to scarring.[5]
The exact criteria for the diagnosis of ABPA are not agreed upon. Chest X-rays and CT scans, raised blood levels of IgE and eosinophils, immunological tests for Aspergillus together with sputum staining and sputum cultures can be useful. Treatment consists of corticosteroids and antifungal medications.[2]